
In the News
Virtual Doctor Visits are Getting more Popular, but Questions Remain About Who Pays
-
Focus Areas
Health Care & Population Health -
Issues
Technology & Telehealth -
Expertise
Technical Assistance -
Programs
Center for Connected Health Policy

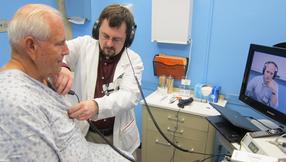 Tucked into the federal budget law Congress passed in February was a provision that significantly expands the use of telemedicine — long a hyped health-care reform and now poised to go mainstream within five to 10 years.
Tucked into the federal budget law Congress passed in February was a provision that significantly expands the use of telemedicine — long a hyped health-care reform and now poised to go mainstream within five to 10 years.
“There’s much broader recognition of the benefits,” said Mei Wa Kwong, executive director of the Center for Connected Health Policy, a research group that promotes telemedicine in Sacramento. “The law is the latest to make telemedicine more accessible. But we still have a ways to go before most consumers are aware of the option.”
The new law allows Medicare to cover telemedicine services for people who have had a stroke and those who get kidney dialysis. It also permits Medicare Advantage plans — private plans that enroll a third of Medicare beneficiaries — to offer telemedicine as a covered benefit.
Separately, as of Jan. 1, Medicare began allowing doctors to bill the government for monitoring certain patients remotely using telemedicine tools — for example, tracking heartbeat and rhythm, blood pressure and blood glucose levels.
Telemedicine, also referred to as telehealth, uses computers to deliver virtual services. In the easiest-to-understand example, a patient in one location has an e-visit with a doctor in another location. They are connected via a secure video link. Proponents say that more sophisticated monitoring is on the horizon and that virtual encounters will become more commonplace.
As acceptance and adoption of telemedicine expands, so does coverage. All private health plans, Medicare, state Medicaid programs and the Department of Veterans Affairs now cover some e-visits. More health centers and hospitals are launching virtual health centers. And websites that offer virtual “doctor-on-demand” services are proliferating.
Concerns exist, however. Doctors worry that they may get paid less if insurance reimbursement is lower for e-visits than for in-person appointments, or that e-visits could undermine the doctor-patient relationship by reducing face time. They point out that for some ailments, such as strep throat, it’s best if the patient sees a doctor or other provider.
Health economists, meanwhile, are concerned that e-visits could add to costs rather than constrain them — if, for example, doctors and patients schedule e-visits unnecessarily because they are quick and easy. Also, insurers may be motivated to push doctors to do more e-visits instead of in-person visits to save money. And for some people, access to proper equipment or Internet access can be difficult.
“The potential for abuse is there,” says Robert Berenson, a Medicare expert at the Urban Institute. “We will need to prevent gaming and misuse of the system. But, generally, helping people avoid unnecessary doctor’s office and hospital visits is a good thing, if we do it right.”
Here’s a briefing on telemedicine basics:
Q: Are e-visits available from most hospitals and doctors?
A: Not yet. But access is increasing. Ask your doctor, clinic or hospital.
In some cities, medical centers are setting up telehealth “hubs” to handle patients. For example, Penn Medicine in Philadelphia launched its Connected Care center in February with 50 full-time employees, 24/7 access to care and a program to treat chronically ill patients at home. Some of the center’s e-visit services are open only to Penn Medicine employees, but other services are available to anyone, with a focus on residents of Pennsylvania, New Jersey, Delaware and Maryland, said Bill Hanson, vice president and chief medical information officer at Penn Medicine.
Similarly, Mercy Virtual in Chesterfield, Mo., a St. Louis suburb, serves patients throughout the Midwest and those treated at Mercy Health’s 44 hospitals in five states. Launched in 2015, Mercy Virtual provided care to 750,000 people in 2017 with a team of 700 doctors, nurses and support staff.
Other medical centers with virtual health programs include Avera Health, based in South Dakota; Cleveland Clinic in Ohio; Dignity Health in San Francisco; Intermountain Healthcare in Utah; and Kaiser Permanente, a managed-care health system in California and elsewhere.
Kaiser Permanente reported last year that 21 percent of its 110 million patient interactions in 2015 were e-visits. Officials there predict that by 2020, e-visits will exceed in-person visits.
Q: What restrictions do health plans, Medicare and Medicaid put on e-visits?
A: Health-plan coverage varies, but most private insurers cover e-visits, and 34 states and the District require that they do. A few states still require that a patient relationship be established with an in-person visit before a provider can bill for an e-visit. Check with your insurer about its policies.
Medicare’s coverage of e-visits is more restrictive. First, e-visits must take the place of an in-person visit. Second, Medicare largely restricts e-visits to those that occur in rural areas that have a shortage of doctors and/or hospitals. And third, most e-visits can’t occur when the patient is at home. They can be done from a variety of other locations, such as a rural health clinic, a dialysis center or skilled nursing facility.
In contrast, almost all state Medicaid programs cover e-visits in the home. But restrictions still apply. For example, only 22 states cover remote patient monitoring for Medicaid enrollees.
The federally funded Telehealth Resource Centers has detailed explanations of e-visit restrictions and limitations.
Q: Do I need special computer equipment?
A: No. E-visits and other forms of telemedicine are done over commonly available computers, laptops, tablets and smartphones, and are typically encrypted to protect privacy. Specialized equipment is usually needed for remote monitoring of blood pressure or heart rate, for example. One vexing barrier: broadband availability in rural areas. Also, millions of low-income and older Americans still lack WiFi in their homes.
Q: What services can I get through telemedicine?
A: Most e-visits are for primary care or follow-up services, such as assessing symptoms or checking on people who have had a medical procedure. But a growing number are for people with chronic conditions who are being monitored at home, said Kwong.
Dermatology e-visits are becoming especially common. You can send a close-up photo of a skin rash, mole or other problem for an immediate assessment. Psychotherapy by e-visit is also expanding.
Originally published by The Washington Post
More Updates
Work With Us
You change the world. We do the rest. Explore fiscal sponsorship at PHI.
Support Us
Together, we can accelerate our response to public health’s most critical issues.
Find Employment
Begin your career at the Public Health Institute.



