Tool: Telehealth Policy Finder
-
Focus Areas
Data, Technology & Innovation -
Issues
Technology & Telehealth -
Programs
Center for Connected Health Policy
Across the country, no two states are alike in how they define and regulate telehealth. To help policymakers, health advocates and other health care professionals understand the policies and trends throughout the nation, the Telehealth Policy Finder tool compiles telehealth-related laws and regulations across all 50 states and the District of Columbia, as well as at the federal level.
Explore the Policy Finder tool
How the FQHCs Have Impacted Medicaid Policy
Federally Qualified Health Centers (FQHCs) provide necessary services for some of the most vulnerable populations. However, due to their unique structure, Medicaid telehealth policies can be very nuanced and complicated.
PHI's Center for Connected Health Policy has created a separate section on its policy finder tool that lists the Medicaid fee-for-services policies on telehealth as they relate to the FQHCs. The topic categories vary slightly from what is found in the rest of the policy finder due to the unique policies that apply to FQHCs, and includes: Definition of visit; Modalities allowed; Same day encounters; Eligible originating site; Eligible distance fee; Facility fee; PSS rate; Home eligible; and Patient-provider relationship.
Explore CCHP's FQHC policy finder to view the policies that exist in your state.

Latest Policy Developments in CCHP’s Telehealth Policy Finder and Policy Trends Map (Updated 4/10/2024)
• California: California Medicaid updated their Telehealth Provider manual to implement two new telehealth provider requirements:
1. Patient Choice of Telehealth Modality – For Medi-Cal providers that do offer telehealth modalities, they must offer Medi-Cal recipients the ability to choose whether they want to receive covered services through synchronous interactive audio/visual telecommunication systems or synchronous, telephone or other interactive audio-only telecommunications systems. Medi-Cal recipients may freely choose and change at any time their desired modality. Medi-Cal providers are exempt from the requirement to offer both telehealth modalities if the Medi-Cal provider does not have access to broadband, but supporting documentation must be available to DHCS upon request.
2. Right to In-person Services – Medi-Cal providers furnishing services via telehealth must also either offer services in-person or have a documented process in place to link Medi-Cal recipients to in-person care within a reasonable time.
• District of Columbia: The Department of Health Care Finance finalized emergency rules that amended billing requirements for Assertive Community Treatment (ACT). The rules define the services that constitute a contact, when telehealth can be used, and establish standards for the types of contacts that a provider must deliver to receive the monthly payment. The rule does allow needs-based assessments to determine service eligibility to be conducted through telehealth. Additional emergency rules adopted expands services for persons with developmental disabilities in the Medicaid Home and Community-Based Services programs and allows the use of remote support services that employ technology. Finally, the Alcoholic Beverage and Cannabis Administration issued a final rule defining and authorizing practitioners to provide telehealth medicine services to qualifying patients, including recommending the use of medical marijuana, consistent with the laws and regulations governing their medical practice.
• Indiana: In response to Indiana House Enrolled Act 1352 (2023), the Indiana Health Coverage Programs (IHCP) has implemented a new telehealth-only provider enrollment for providers that wish to perform only telehealth services (with no physical site where patients are seen) and that meet the Indiana licensure and other special requirements outlined in this bulletin. This telehealth-only provider enrollment option is currently available on the IHCP Provider Healthcare Portal.
• Nevada: Nevada Medicaid updated their Telehealth Manual to remove a limitation on audio only telehealth for behavioral health delivery that limited it to targeted case management and crisis intervention services. The manual now states that audio only is allowed in circumstances where there is medical necessity and its appropriateness for the recipient is documented in the medical record.
• New York: Medicaid issued an Update in January announcing that they would reimburse for eConsults effective April 1, 2024. Additionally, S 8058 was passed which defines gender-affirming care, and added the definition to sections of law applicable to providers prescribing abortion medication to out-of-state patients by means of telehealth.
• North Carolina: North Carolina Medicaid updated their Dental Services manual in December to add coverage for both synchronous and asynchronous dental services for specific codes. See manual for list of requirements. Additionally, the Traumatic Brain Injury Appendix K Flexibilities were also updated to note that members could access Life Skills Training, Cognitive Rehabilitation, Day Supports, Supported Employment, Supported Living, Community Networking via telehealth. The guidance specifies that the use of telehealth shall not exceed 25% of the authorized service hours per week (i.e. if an individual is authorized 40 hours a week, the individual may use the real time two-way interactive audio and video telehealth 10 hours per week).
• Oregon: Amended a regulation on their Medicare Assistance out-of-state services policy to specify that they do not provide payments for items or services to any financial institution or entity located outside of the United States, which effectively prohibits payments to telemedicine providers and pharmacies located outside of the United States. A separate regulation was also amended to stipulate that a license is not required of a physician or physician assistant when they are located outside the state and have an established provider-patient relationship with a patient in Oregon temporarily for the purpose of business, education, vacation or work who requires the direct medical treatment by that physician or physician assistant; or in circumstances where a patient located in Oregon requires temporary or intermittent follow-up care from a physician or physician assistant with whom they have an established provider-patient relationship.
• Washington: Washington State Health Care Authority (Medicaid) updated their Telehealth Manual to include best practice in conducting telemedicine services to include asking a client if they need assistive devices to participate in virtual care, include accessibility options within a telehealth program and use technology designed with equity in mind. Washington Medicaid also updated their physical health audio-only procedure code list to remove, revise and add specific codes effective Jan. 1, 2024. Amendments were made to Medicaid coverage of home health services via telemedicine and SB 5821 was passed to align established relationship requirements related to audio-only access across statute (see State Legislation section of newsletter below). Likewise, Permanent rules were adopted by the Office of the Insurance Commissioner updating audio-only established relationship requirements. Additional legislation approved includes: HB 1939 which enacts the Social Work Compact in Washington; SB 5481 which provides allowances for out-of-state providers and requires the review of the Uniform Law Commission’s proposal regarding implementing a process for out-of-state provider registration within state boards, and SB 5983 which allows medical assistants with telehealth supervision to provide intramuscular injections for syphilis treatment.
Fall 2023 Updates
During their Fall review, CCHP noted that many state Medicaid programs moved to add a range of specific services as reimbursable when delivered via telehealth as well as additional provider types that can serve as distant site providers. For instance, Nebraska Medicaid released guidance incorporating many PHE policies into their permanent reimbursement policies. This includes reimbursement for services such as health check services, mental health and substance use, physical and occupational therapy, physician services, speech pathology and audiology, visual care, and chiropractic services. Moreover, various Medicaid programs have adopted strategies reminiscent of Medicare, detailing eligible telehealth service codes in a list for providers to reference, with some states identifying a subset of the codes as suitable for audio-only interactions. Likewise, many states have also now adopted the place of service (POS) code system previously introduced by Medicare, where POS 10 indicates services provided at a patient’s home and 02 indicates telehealth services provided at an originating site other than the patient’s home.
Just as in previous issues of this Summary Report, since the onset of the COVID-19 PHE, state Medicaid programs continue to expand their audio-only reimbursement policies. However, the transition to permanent policy changes has typically been characterized by a more deliberate and cautious approach compared to the rapid implementation of temporary measures during the COVID-19 pandemic. North Dakota’s General Information Provider Manual was updated, for instance, to provide for reimbursement of audio-only telephone evaluation and management (E/M) services, but only when initiated by an established patient or guardian of an established patient. In June, Vermont Medicaid issued a Banner Notice related to their coverage of audio-only services, announcing that they will continue to allow audio-only services for a defined list of codes, which mirrors the Medicare list of codes. In addition to audio-only telephone, a limited number of states are expanding into other modalities including store-and-forward and remote patient monitoring. For example, Utah provides reimbursement for interprofessional internet assessment and management services for psychiatrists, which are listed as covered in their provider manual. Meanwhile, Texas passed HB 2727 which amends the statute related to its home telemonitoring services to modify the program to allow FQHCs and RHCs to be eligible providers. It also adds end stage renal disease or a condition that requires renal dialysis treatment to the list of eligible conditions for remote telemonitoring services, among other changes.
Policies addressing requirements for provider enrollment, including rules around an in-state address, is the newest phenomenon in Medicaid telehealth policy. Alabama’s Telemedicine Policy, for instance, now requires an in-state or qualifying bordering state site of practice address from which telemedicine services can be provided. In some states, this has become such an issue that it necessitated legislation (for example, Indiana’s HB 1352), forbidding Medicaid programs from requiring an in-state address or provider’s presence for Medicaid enrollment.
Read the full Fall 2023 report, and explore the state summary chart showing where states stand on many key telehealth policies, as well as an infographic highlighting key findings.
Additional findings:
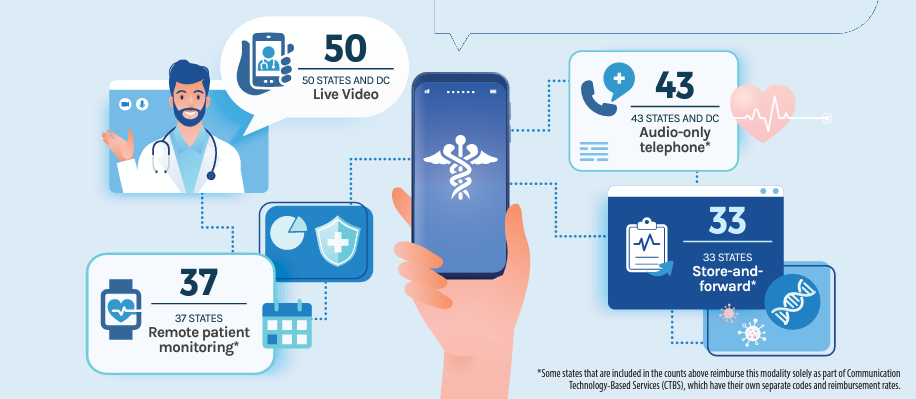
- Fifty States and Washington DC provide reimbursement for some form of LIVE VIDEO in Medicaid fee-for-service. Both the jurisdictions of Puerto Rico and Virgin Islands do not explicitly indicate they reimburse for live video in their permanent Medicaid policies.
- Thirty-three state Medicaid programs reimburse for STORE-AND-FORWARD. Florida, Montana, North Dakota, South Carolina and Utah are the states which added reimbursement for store and forward, although each in a limited capacity, and some only through specific communication technology-based service (CTBS) codes since the Spring update.
- Thirty-seven state Medicaid programs provide reimbursement for REMOTE PATIENT MONITORING (RPM). Three states, (Florida, Idaho, and Iowa) added reimbursement for RPM since Spring 2023.
- Forty-three states and DC Medicaid programs reimburse for AUDIO-ONLY telephone in some capacity; however, often with limitations. Seven states including Alabama, Idaho, Kansas, Montana, Nebraska, Oklahoma, and Vermont added reimbursement for audio-only telehealth in some capacity since Spring 2023.
- Twenty-five state Medicaid programs including Alaska, Arizona, California, Hawaii, Illinois, Iowa, Kentucky, Maine, Massachusetts, Maryland, Michigan, Minnesota, Missouri, New York, North Carolina, North Dakota, Ohio, Oregon, South Carolina, Texas, Utah, Vermont, Virginia, Washington, and Wisconsin reimburse for ALL FOUR MODALITIES (live video, store-and-forward, remote patient monitoring and audio-only), although certain limitations may apply.
- Forty-three states, the District of Columbia and Virgin Islands have a PRIVATE PAYER LAW that addresses telehealth reimbursement. Not all of these laws require reimbursement or payment parity. Twenty-four states have explicit payment parity. No new states have added a private payer law since Spring 2023, though a few states have made modifications to private payer law requirements.
- Thirty-six states and DC explicitly allow FQHCs to serve as originating sites and thirty-seven states and DC explicitly allow FQHCs to serve as distant sites for telehealth. Meanwhile, twenty-five state Medicaid programs and DC explicitly clarify that FQHCs are eligible for the prospective payment system (PPS) rate when serving as distant sites.
Getting started with the Policy Finder
Launched in Spring 2021 by PHI’s Center for Connected Health Policy (CCHP), the Policy Finder tool is a searchable, easy-to-use database that is updated consistently throughout the year. Formerly known as the State Telehealth Laws and Reimbursement Report, the information from the online database can be exported for each state into a PDF document using the most current information available on CCHP’s website.
Use the Policy Finder tool to:
- Look up telehealth-related laws and regulations by topic, including COVID-19, Medicaid & Medicare, Private Payer and Professional Requirements
- Explore all current laws, temporary COVID-19 actions, and pending legislation in all 50 states and the District of Columbia, as well as at the federal level
- Compare the policy of any of the topic areas for any two states
- View color-coded maps recapping policy trends by state across topic areas, including Medicaid reimbursement for live video, store and forward and remote patient monitoring
The Policy Finder is designed to provide timely policy information that is easy for users to navigate and understand. Watch a quick tutorial to explore the tool, see how to use it and learn about its features:
Please note: this information should not be construed as legal counsel. Consult with an attorney if you are seeking a legal opinion.
Originally published by Center for Connected Health Policy
Work With Us
You change the world. We do the rest. Explore fiscal sponsorship at PHI.
Support Us
Together, we can accelerate our response to public health’s most critical issues.
Find Employment
Begin your career at the Public Health Institute.