
In the News
To Reduce Harm, Some Bay Area Venues Are Providing Fentanyl Testing Strips
- KQED
-
Focus Areas
Alcohol, Tobacco, Drugs & Mental Health -
Expertise
Health Education & Promotion -
Programs
CA Bridge -
Strategic Initiatives
Opioids
Almost a year has passed since Crisis Club Gallery, a community space in Oakland, opened its doors, something that makes co-owner Niko Nada very proud.
“It took a few months of getting a bunch of kids who didn’t know about construction to do construction,” Nada said. “We built all these walls, we laid everything.”
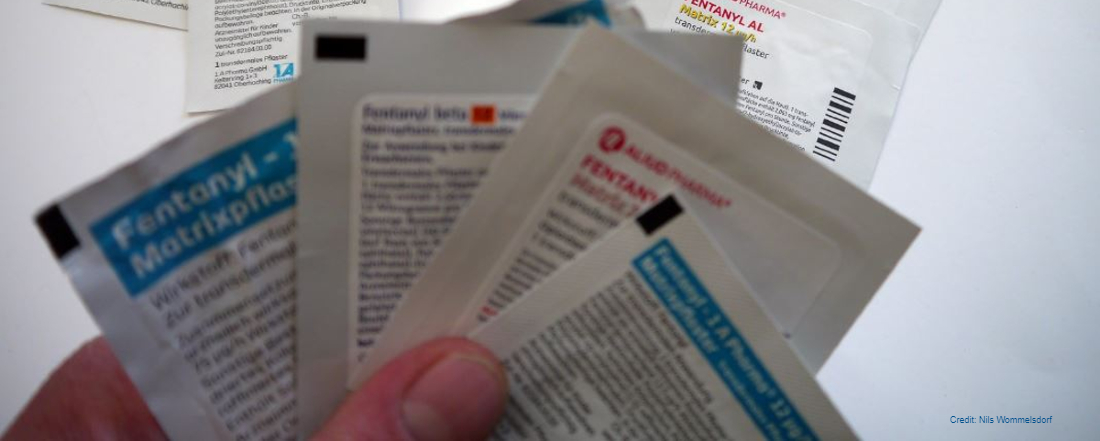
Among other things, the group set up a shelf in the bathroom with a supply of fentanyl testing strips — small pieces of paper that can be used to identify whether a substance contains fentanyl. Anyone who comes into the gallery can take as many strips as they need.
On the shelf are also safe snorting and injection kits, and other products meant to help people who use drugs do so in the safest way possible.
Hospitals, health clinics and emergency departments are making these supplies available, too. But according to Nada, venues like galleries and bars can play a big role in increasing the rate of testing.
“[Business owners] have the resources to have a space that can be an influence,” said Nada, whose gallery receives testing supplies through a network of friends.
The highly addictive synthetic opioid fentanyl is about 50 to 100 times more potent than morphine. It is often mixed with other drugs, like ketamine, ecstasy, cocaine and heroin to increase potency.
Fentanyl testing strips are easy to use and effective, explained Dr. Hannah Snyder, an assistant professor at UCSF and director of the California Bridge program, which focuses on providing health care for people who use drugs.
When people want to use fentanyl testing strips, she said, “they can take a tiny amount out of whatever their drug is. Maybe it’s the edge off of a pill or residue.” That residue can then be mixed with a small amount of water and dipped in the testing strip. After a few minutes of drying, if two lines appear, that signifies a negative result. Just one line, however, means there is likely some trace of fentanyl in the other drug. Testing also allows people to make the decisions that can help reduce harm, she added.

It's not a perfect test, but that's really important so a person can say, 'This is a drug that I think is too high-risk for me to take,' or 'This is a drug that I want to take with other people around me to make sure I'm safe.'Dr. Hannah Snyder, CA Bridge
What can be done to prevent an overdose from turning fatal?
Fatal opioid overdoses can be prevented with a drug called naloxone (also known by the brand name Narcan), which temporarily attaches to opioid receptors and reverses and blocks the effects of other opioids. According to the National Institutes of Health, naloxone very rarely causes any serious side effects.
A number of Bay Area counties, including San Francisco and Santa Clara, provide free naloxone/Narcan kits and training for how to use them and for how to recognize signs of an overdose.
Pharmacists in California also are permitted to provide naloxone without a doctor’s prescription.
Additionally, medication-assisted treatment for opioid addiction is widely available. Emergency doctors can prescribe FDA-approved drugs that treat opioid dependence and can arrange for patients to follow up at outpatient centers.
What are common signs of an overdose?
Someone may be overdosing if they’re acting groggy and lethargic or are barely able to stand, and if slow breathing grows irregular or even stops altogether. Very constricted pupils in someone’s eyes — known as “pinpoint pupils” — that don’t expand when exposed to light also are a common sign of an overdose.
Click below to read the full story from KQED.
Originally published by KQED
More Updates
Work With Us
You change the world. We do the rest. Explore fiscal sponsorship at PHI.
Support Us
Together, we can accelerate our response to public health’s most critical issues.
Find Employment
Begin your career at the Public Health Institute.



