Tool: Tracking COVID-19 Related Telehealth State Actions
-
Focus Areas
Communicable Disease Prevention, Health Care & Population Health -
Issues
Technology & Telehealth -
Programs
Center for Connected Health Policy -
Strategic Initiatives
COVID-19
PHI’s Center for Connected Health Policy (CCHP) has developed a tool to track the emergency actions and legislation directly resulting from the COVID-19 pandemic.
Get started with the tool
Since state Governors declared states of emergency in mid-March, Medicaid programs have released a multitude of documents pertaining to waivers and easing of restrictions related to telehealth. Common temporary allowances found in the Medicaid documents include:
- Allowing the home to be an originating site for telehealth
- Expanding the types of providers allowed to be distant site providers during a telehealth interaction
- Providing reimbursement for additional types of services when delivered via telehealth
- Allowing the telephone as a mode of service delivery
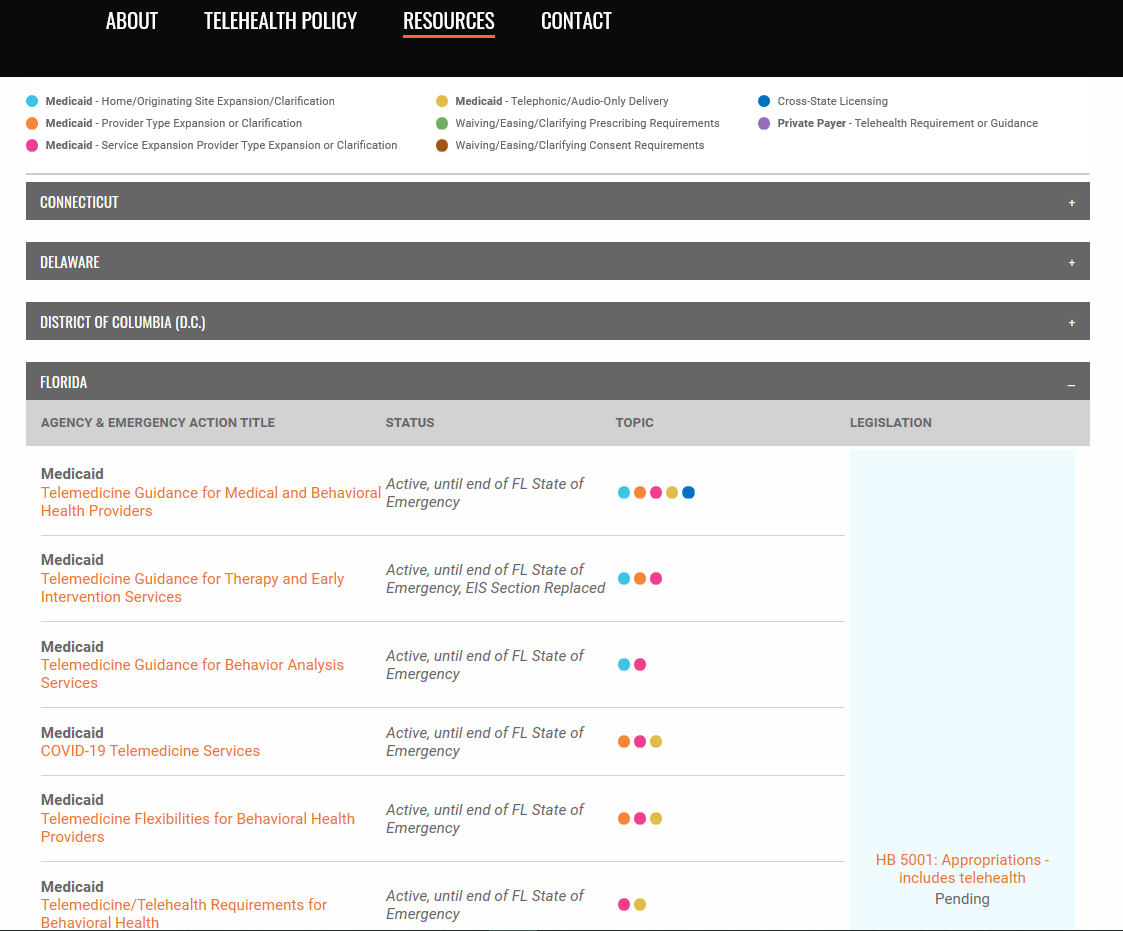
In addition to the above, most state Departments of Insurance have released either guidance or provided temporary requirements for health plans in their state to cover telehealth delivered services sometimes mandating payment parity with in-person services. Medical Boards have also in some cases eased cross-state licensing, consent and prescribing requirements for telehealth delivered services on a temporary basis during the state of emergency. CCHP has identified in its tool which documents address each of the above described topic areas, along with their corresponding expiration date, if available.
The sources used to gather the list of state actions include each state’s Office of the Governor (which often includes executive orders), Medicaid Program, Medical Board and/or Department of Insurance. CCHP plans to update this tool on a regular basis so that the current telehealth waivers and guidance documents are all in one place and can be tracked as they are either extended in duration, altered, expire or made permanent.
If you have additional information on state actions that are not included in CCHP’s state action tool, please submit your information to info@cchpca.org.
Originally published by Center for Connected Health Policy
Work With Us
You change the world. We do the rest. Explore fiscal sponsorship at PHI.
Support Us
Together, we can accelerate our response to public health’s most critical issues.
Find Employment
Begin your career at the Public Health Institute.

